


Bridging hospitality and healthcare
Photos by Ashley Barnas December 07, 2022
UD’s Patient Experience Academy improves trust between the Wilmington VA and veterans
When a person is told they have a life-threatening illness, they won’t hear anything else.
But what a doctor or medical provider says next is pivotal. That’s where empathy comes into play.
“The doctor or the medical provider must really stop and ask questions of the patient: what are they thinking? What are they feeling? And really build that relationship,” said Sheryl Kline, deputy dean and Aramark Chaired Professor in the University of Delaware’s Alfred Lerner College of Business and Economics.
Some people possess empathy naturally while others need time and space to develop it. That’s one intricate piece of the all-encompassing Patient Experience Academy, an interdisciplinary collaboration between UD’s Lerner College, the College of Health Sciences, the College of Arts and Sciences, Academic Technology Services, and the Division of Professional and Continuing Studies.
“The foundation of empathy is in being an active listener and really focusing on what the person is saying to you. To be empathetic, you must be vulnerable, and for a lot of people that’s very hard to do,” Kline said. “In our classes, we practice and provide space so that someone can be vulnerable. We work on how you talk, really sit with a patient so that they know you’re on their side and help them develop the skills and behaviors that help the patient.”
Twenty-seven years ago when registered nurse Laura Selwood first began working in healthcare for the U.S. Department of Veterans Affairs (VA), empathy wasn’t a focus.
“Now, when a veteran has an issue regardless of whether it involves primary care, the buck stops here. I tell them: ‘I’m sorry you’re having this problem, or I’m sorry this is happening to you. I can see this is frustrating. Let me help you.’ That validation of their feelings is important,” Selwood said.
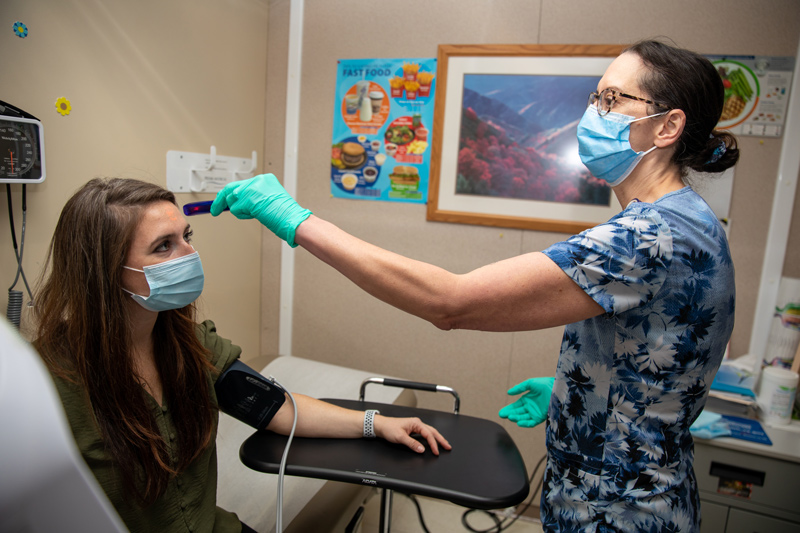
Registered nurse Anne Anyanga, who has worked with the VA for more than three years, has learned calming tactics and enhanced her communication skills.
“The training has given me an opportunity to reflect on how we deliver care and how we use our values as an organization to show that we really do care,” Anyanga said. “We treat veterans for a variety of mental health conditions based on their past experiences, and I’ve learned how to lower the temperature when they’re upset. I used to keep quiet, but I’ve learned your tone matters in how you interact with them and resolve their issues.”
Both learned that in the Patient Experience (PX) Academy, which was born in 2014 and first launched with ChristianaCare, where 1,000 staff and medical providers were trained in hospitality healthcare. The pillars of the PX Academy are based on managing changing expectations, excellent customer service, service recovery, openness to experience, comprehensive listening and empathy.
“The program drove ChristianaCare’s patient experience scores over the 90th percentile as measured by more than 8,000 patients who responded to the surveys. This level of achievement is the goal for almost every healthcare organization,” said Ali Poorani, the academy’s faculty director and principal investigator, who’s also an associate professor of hospitality business management in Lerner.
Based on the success of the program, the Wilmington VA approached the University in 2018, seeking to bring the PX Academy to its healthcare system with the curriculum tailored to meet the needs of the VA’s unique population.
“The VA is very conscious that veterans sacrificed for our country and to give us freedoms, and so our program focuses on taking care of veterans and their unique needs,” Kline said. “We’re helping the people who help the veterans, and these healthcare providers are doing more than just providing medical care. Many veterans have profound and emotional experiences, and so the training focuses on emotional aspects as well.”
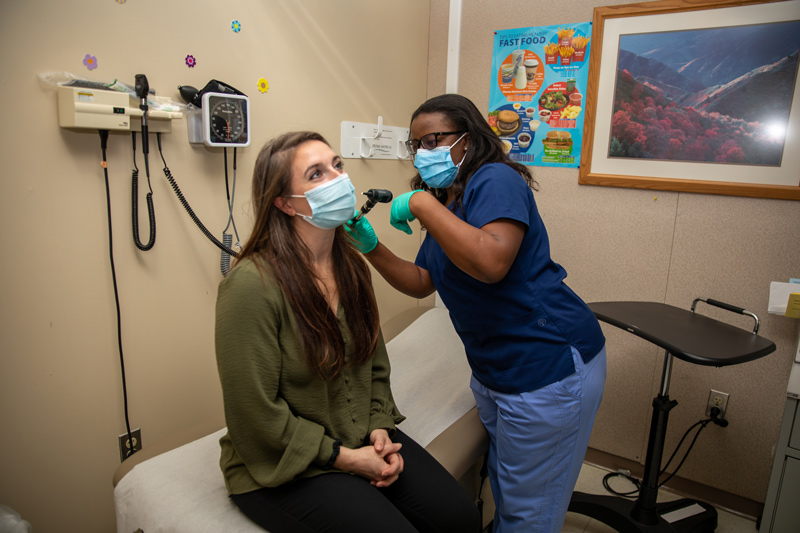
Vincent Kane, director of the Wilmington Veterans Affairs Medical Center, said one of the center’s strategic initiatives is to improve trust between the medical center and the veteran community, putting veterans and their families first – and what matters to them – at the forefront.
“Having the veteran’s voice at the center of our relationship and how and where we deliver healthcare is critical,” said Kane. “When you define exceptional healthcare, you must ensure that it’s research-informed, evidence-based and state-of-the-art, but it also has to be delivered in a caring, compassionate and respectful way. If you don’t have both, then you don’t have exceptional healthcare. To work with UD to build up the hospitality component of healthcare delivery to improve the overall veteran healthcare experience was just a great marriage.”
The VA Patient Experience Academy launched initially with managers and saw astounding results.
“After the first phase of training nearly 400 medical providers at the Wilmington VA Medical Center and five satellite locations, the results as measured by veterans were outstanding, outperforming national averages by about 2.5%. That was a huge improvement,” Poorani said. “They also became number one in terms of patient experience in Delaware — better than other healthcare systems, so that’s something we really are proud of.”
Kane is proud of the center staff’s efforts to improve the veteran’s overall experience, but knows more work is needed, noting the VA must constantly innovate and improve.
“All of our metrics went up dramatically, including how the veterans perceived their provider,” Kane said. “But these training sessions can’t be a one-and-done. They must be hardwired into how we help and support our staff during onboarding.”
While the program was paused during the COVID-19 pandemic, its success spawned a new two-year contract between UD and the Wilmington VA. A reimagined virtual program launched in October in large part due to an online platform designed and developed by Kelly Cross and Paul Hyde of Academic Technology Services, who continue to support facilitators of the VA PX Academy. The twice-weekly entirely virtual training will reach as many as 700 Wilmington VA employees in the region, including doctors and nurses.
The interactive interprofessional education program creates a bridge between hospitality and healthcare and involves the dynamic Healthcare Theatre program, a joint venture between CHS and CAS.
“From a human-centric perspective, we need to be mindful that patients are human first and a patient when they seek out healthcare,” Poorani said. “But after they leave the hospital or the primary care office, they’re also consumers. So, they are seeing a lot of things happening as a consumer in other industries, and they expect that from their healthcare.”
Healthcare Theatre trains students to be patients and family members, who then take part in simulated healthcare encounters, so learners can practice their medical and communication skills in safe, but highly realistic, healthcare encounters.
By incorporating Healthcare Theatre in the PX Academy curriculum, providers are placed in challenging situations, and instructors observe how they react to patients. Allan Carlsen, director of Healthcare Theatre, said he and other instructors are watching for certain things.
“We want to make sure that doctors introduce themselves well, present a plan of care, and ask the patients if they understand it and accept it,” Carlsen said. “These scenarios give providers an opportunity to practice what’s being taught — empathy, advocacy, all the communication skills, and service recovery. When things go south in these interactive freeze-frame encounters, the providers can stop and start the simulation and talk among themselves. The doctors have an opportunity to help two different vets, each with varying issues, and they get to practice talking to them.”
One “tougher” scenario Selwood and Anyanga faced included a veteran from out-of-town coming in for care with a family member with no medical information.
“That scenario helped us learn how to coordinate care and interact with our veterans to instill confidence that the VA really is a nationwide healthcare system,” Anyanga said.
Selwood said that scenario encouraged her to change her approach with new patients and their families.
“Previously, I used to have loved ones contact eligibility with their questions,” Selwood said. “Now, I’m equipped with more knowledge and can make contacts directly for them and provide better service connections, helping them feel more empowered.”
Poorani said through the PX Academy, the faculty and VA staff are bridging hospitality and healthcare.
“Though hospitals are not hotels, our investigations show nearly 70% of what hospitals do is rooted in hospitality,” said Poorani.
The success of the academy is data-driven and based on numeric and comment-based pre-and post-assessments provided by VA staff.
William Sullivan, adjunct faculty at Lerner and managing director of the Courtyard by Marriott – Newark University of Delaware, said the academy’s success relies strongly on data, and that data, thus far, “has told a great story.”
“This is exactly what we do in the hospitality world,” Sullivan said. “When we marry the concepts together, there’s a lot of great positives. But most of our guests come in healthy, and unfortunately, in the VA’s case many come in with illness. So, we must be different, but we also apply some of the same tools to the measurement process.”
All VA Wilmington staff will ultimately undergo training in the VA PX Academy which brings comfort to Selwood and Anyanga.
“The care starts in the call center, when a veteran or their loved one makes that first call and the first words and the tone that they hear: ‘Hello, how can I help you?’” Anyanga said. “By the time they get to a nurse, I could be the third person they’re talking to, so it’s beneficial that we’re all on the same page in care delivery.”
Paul Weaver was a senior chief petty officer in the U.S. Navy. He retired in 1992 after 23 years of service and uses the VA healthcare system. He’s now an actor with UD’s Healthcare Theatre Program and called the program a “natural application” to fix some of the issues he’s seen first-hand.
“It gives me hope that the next time I go to the VA, things may be different,” Weaver said. “The caregivers and staff must realize how important they are to the veteran. They depend on VA employees to solve their problem, and employees must realize they have a responsibility to provide a solution or seek the answer to the veteran’s problem. Even if they can’t provide a solution for every veteran that walks through the door, they must satisfy them, so they don’t walk away feeling defeated or ignored.”
Contact Us
Have a UDaily story idea?
Contact us at ocm@udel.edu
Members of the press
Contact us at 302-831-NEWS or visit the Media Relations website

