


Focusing on musculoskeletal research
Illustration by Jeffrey C. Chase | Video courtesy of Dawn Elliott and Elise Corbin March 17, 2021
UD wins NIH grant for new center with female professors leading the way
A pulled muscle, an aching joint. Regrettably, it’s an experience we can all relate to — from the youngster with the sprained ankle, to the centenarian with gnarled fingers throbbing from arthritis, to that excruciating moment when you threw your back out doing yard work.
According to the U.S. Bone and Joint Initiative, in 2015 alone, more than half of all Americans reported having a musculoskeletal condition — more than any other medical problem — and the number likely won’t be getting any smaller as the U.S. population ages. The number of Americans age 65 and older is expected to more than double over the next 40 years.
“It’s a really big problem,” said Dawn Elliott, Blue and Gold Distinguished Professor of Biomedical Engineering at the University of Delaware. “Having painful joints doesn’t necessarily kill you, but it can ruin your life.”
Elliott is now leading a major initiative to help tackle the problem. She has won an $11.8 million grant from the National Institutes of Health to establish the Delaware Center for Musculoskeletal Research — an NIH-designated Center of Biomedical Research Excellence (COBRE).
From tendonitis to osteoarthritis, the center will focus on uncovering what happens at the cellular level when injuries and inflammation occur and will test potential therapeutic interventions. This basic science and preclinical research will complement clinical work underway at UD’s top-ranked physical therapy program, the Delaware Rehabilitation Institute and Delaware Center for Translational Research, creating a comprehensive basic-to-clinical research pipeline aimed at powering down these painful disorders.
“We congratulate Professor Dawn Elliott and her team for this groundbreaking initiative to help ease the suffering of millions of people,” said UD President Dennis Assanis. “The work of this new center will drive discoveries and advancements in treating muscle, bone and joint disorders. It will also deliver fundamental research findings to UD’s nationally recognized clinical programs in physical therapy and rehabilitation, thus playing a critical role in enhancing patient care and student education.”
A center with an innovative approach
Your musculoskeletal system is remarkable, encompassing 206 bones to provide support, moveable parts like cartilage that allow joints to slide, and ligaments and tendons that tie together the bones and 600 muscles. All together, these tissues support your weight, maintain your posture and enable you to move about. And when any single part of this dynamic system gets injured or inflamed, it can affect your entire body.

According to Elliott, making progress in research requires examining this complex system as an integrated whole and at many different scales, all the way down to the microscopic level.
“The mechanics and biology of the musculoskeletal system are inextricably intertwined and long-ranging, affecting each other across multiple scales,” she said. “Mechanical forces at one site affect all the tissues in the kinetic chain, including physical cues in cells and molecules. Biological signal transmission also is long-ranging — when a ligament is damaged, for example, the inflammatory molecules and metabolites released affect the cartilage and bone locally, as well as the surrounding muscles, and even distant tissues such as the cornea.”
The center’s three major aims will be to accelerate fundamental research by supporting innovative multidisciplinary projects, to establish a Multiscale Assessments Research Core with state-of-the-art tools, and to amplify the impact of musculoskeletal research through faculty mentoring, expansion and retention.
Elise Corbin, assistant professor of biomedical engineering, will lead the center’s first project, on sepsis. This extreme response to an infection triggers a chain reaction in the body, damaging tissue, shutting down organs and, without prompt medical treatment, ending in death.
Survivors of sepsis have an increased risk of developing persistent muscle weakness. Although resistance training is widely accepted for rebuilding muscle mass and strength, recent studies suggest that early physical therapy post-recovery may preserve muscle fiber, but not strength.
Corbin will create an innovative 3D microtissue model from human muscle cells to capture impairments and muscle wasting over time in response to inflammatory agents and determine the recovery of contractile function in response to resistance training.
“Ultimately, we hope to positively impact future treatment and improve the quality of life of post-sepsis survivors,” Corbin said.
A legacy of leadership
Joining Elliott in leading the major components of the center will be Professor Velia Fowler, chair of UD’s Department of Biological Sciences, who will co-direct the center; and Professors Millie Sullivan and Liyun Wang, both from the College of Engineering, who will co-direct the center’s Multiscale Assessments Research Core.
The fact that four women will hold all key leadership roles in the center underscores the legacy of success of a previous COBRE focusing on osteoarthritis, which Thomas Buchanan, George W. Laird Professor of Mechanical Engineering, directed.
“That COBRE had a strong mentoring program to foster the development of women biomedical researchers at UD, and several members of our new center’s team, including myself and Professor Wang, participated in it,” Elliott said. “It’s been inspiring to see the impact it has had on women’s leadership and UD’s research community at large.”
Since joining the UD faculty in 2019, Fowler has launched a mentoring program for faculty in the Department of Biological Sciences, where several assistant professors recently have won prestigious NIH R01 grants.
“Similarly, at the new center, we have a deep commitment to mentoring and career development to support the transition of junior faculty to extramurally funded research investigators,” Fowler said. “This is absolutely essential in cultivating and retaining new biomedical research leaders. We are fortunate to have the UD ADVANCE Institute at the University, which will serve as a critical collaborator and faculty resource.”
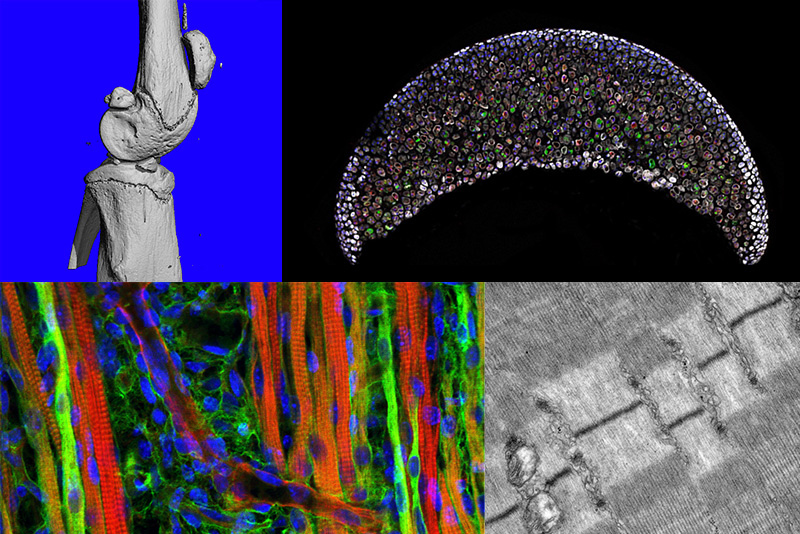
On the technology side, new scientific instruments and techniques, from in vivo micro-computed tomography to photoacoustic imaging systems to customized biomechanical manipulation systems, will allow researchers to investigate the interactions of cells and tissues with their environment. These state-of-the-art tools will be the domain of the Multiscale Assessments Research Core, under the leadership of Sullivan and Wang. The core will be located in newly renovated space on the second floor of the Life Sciences Research Facility.
"This research core will serve not only as an intellectual hub for the DCMR community, but also as a gateway to access other superb partner cores such as UD’s Bio-Imaging Center," Wang said.
The COBRE funding also will expand and reorganize the staffing model for core resources relevant to the center’s work, including increased support for experimental design and execution.
"The organization of experimental resources and staff under the core umbrella will create a single starting point for our scientists to obtain scientific and technical guidance involving biomechanical, biophysical and bioimaging analysis of musculoskeletal tissues, and it will enable experimental approaches to be refined, validated, codified and shared more broadly," Sullivan said.
With more than 60 researchers working in musculoskeletal and rehabilitation science across the University, UD is a growing force in the field. The Delaware Center for Musculoskeletal Research will serve as a catalyst for further developing a nationally recognized network of researchers dedicated to improving musculoskeletal health.
“These disorders can have a devastating impact on lives,” Elliott said. “Through our studies, we will be working to understand how tissues function, how they break down with aging and injury, and how they heal. Ultimately, we want people to have the ability to take care of themselves, to live without pain and to enjoy an active lifestyle.”
Contact Us
Have a UDaily story idea?
Contact us at ocm@udel.edu
Members of the press
Contact us at 302-831-NEWS or visit the Media Relations website

