The Parkinson's Clinic
STAR Campus clinic provides individualized care for people with Parkinson's disease
1 p.m., April 1, 2014--Bill Smith sat on the examining table and answered his doctor’s questions about his symptoms and his medication record. The two discussed Smith’s tremors, gait problems, fatigue, difficulty sleeping, and occasional forgetfulness.
The clinic visit was fairly typical for a person with Parkinson’s disease except that Smith was in an exam room at the University of Delaware’s Nurse Managed Health Center (NMHC), while his physician, Dr. Ray Dorsey, was more than 300 miles away in Rochester, N.Y.
Campus Stories
From graduates, faculty
Doctoral hooding
Dorsey, a neurologist at the University of Rochester Medical Center, is using telemedicine to bring his expertise in movement disorders to Delaware, a state with no specialist in this area.
He is now part of a team at The Parkinson’s Clinic at UD, which provides individualized treatment and care to people with Parkinson’s. Other team members include nurse practitioners, physical and speech therapists, exercise physiologists, nutritionists, and mental health professionals.
Parkinson’s disease affects as many as a million Americans, about 2,000 of them living in Delaware. There is currently no cure for the disease, which affects the nerve cells in the brain that produce dopamine, a neurotransmitter that plays a vital role in movement, emotional responses, and cognition.
The clinic at UD was developed by Ingrid Pretzer-Aboff, associate professor and a recognized scientist and clinician in the national and local Parkinson’s communities, and Allen Prettyman, assistant professor, nurse practitioner and NMHC director.
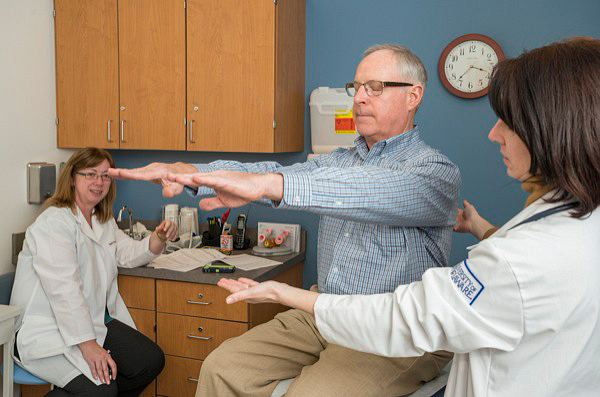
Smith was the first patient to visit the clinic the day it opened at the NMHC’s new facility on UD’s Science, Technology and Advanced Research (STAR) Campus. His appointment began with a routine physical exam by nurse practitioner Beatrice Gaynor, who checked his height, weight, blood pressure, and vision.
Under the watchful eye of Pretzer-Aboff, Gaynor, who is also a Ph.D. student in UD’s nursing science program, then administered a battery of movement, coordination and balance tests.
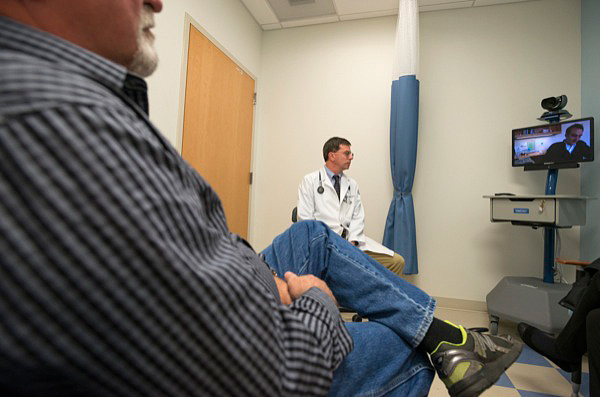
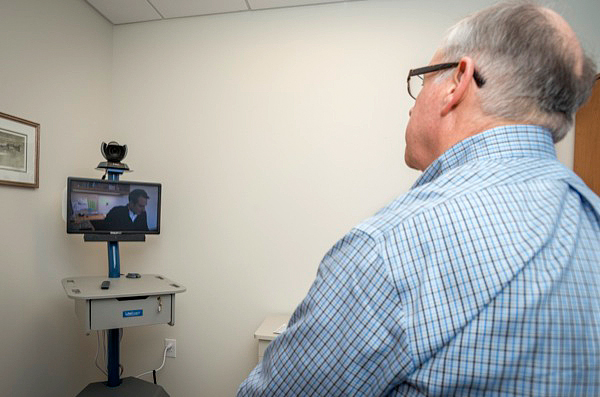
Finally, via the clinic’s telemedicine station, Smith “met” with Dorsey, who will share his findings and recommendations for Smith’s treatment with his local health care team.
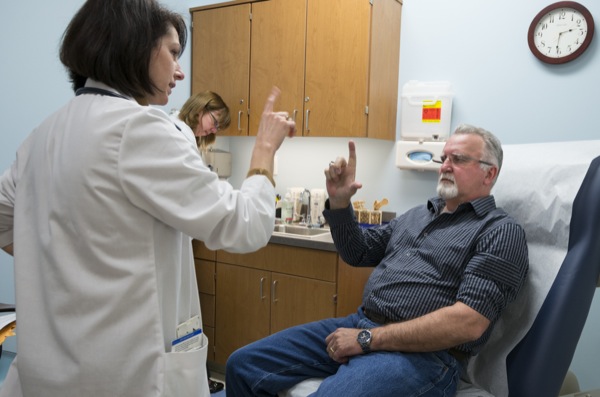
While Smith was meeting with Dorsey, Gary Chard began his intake appointment with the same exams Smith had undergone an hour earlier. Through a set of coincidences, Chard had been diagnosed by Dorsey six years earlier. Chard later moved to Delaware and learned about the clinic at UD through his work with Parkinson’s support groups and research advocacy organizations.
Chard believes in the power of exercise to fight the disease, so he started a running program and completed a 10K run last October. “I firmly believe that the exercise component has softened my symptoms and improved my outlook,” he says.
The primary drugs used to treat the symptoms of Parkinson’s tend to work well at first but lose their effectiveness over time, requiring higher doses with increased side effects. For now, Chard has been able to minimize his use of medication, and he plans to continue working with his healthcare team to determine the best course of treatment for him.
“Individualized care is a hallmark of The Parkinson’s Clinic,” says Prettyman. “Every person we see has different needs, and our goal is to bring a team approach to meeting those needs.”
The Health Sciences Complex at UD’s STAR Campus is facilitating the multidisciplinary care offered to people with Parkinson’s in the new clinic.
Just down the hall from the NMHC is the Delaware Physical Therapy Clinic, a state-of-the-art facility that includes a harness system to provide safe gait training for people with movement disorders caused by Parkinson’s, stroke, and traumatic brain injury.
Exercise physiologists are also weighing in with research findings at UD. Chris Knight, associate professor in the Department of Kinesiology and Applied Physiology, is studying how the nervous system controls movement, and he is conducting experiments to help guide exercise recommendations for older adults and people with Parkinson’s disease.
In another research project, Pretzer-Aboff is part of a team working on the PDShoe, an ordinary beach shoe equipped with force sensors and a vibration system that shows promise for managing “freezing of gait” in people with Parkinson’s. Pilot tests have shown good results with the shoe, and it has enabled the researchers to collect a wealth of data that will be valuable in directing future research, evaluating patients and shaping new therapies.
Pretzer-Aboff has also conducted research on the effectiveness of a community-based exercise program for people with Parkinson’s. The program, based at Beebe Medical Center in Sussex County, Del., was continued by the community even after the research project was completed.
In addition, Barbara Habermann, Nannie Longfellow Professor of Nursing Science at UD, is working in a number of areas related to Parkinson’s disease, including quality of life and end-of-life care for people and their family members.
“I think we have a lot of expertise in the area of Parkinson’s disease,” says Pretzer-Aboff. “Now, through our partnership with Dr. Dorsey and the telemedicine technology, we’ve really added to our ability to provide holistic care to people with Parkinson’s. This was something that was really needed in our state.”
To learn more about The Parkinson’s Clinic or to make an appointment, visit the NMHC website or call 302-831-3195.
The Parkinson Council, Highmark Foundation, and the state of Delaware have provided financial support to The Parkinson’s Clinic.
About The Parkinson’s Clinic
The Parkinson’s Clinic uses cutting-edge telehealth equipment linked to a high-end, Internet-based video network housed in the University of Delaware’s computing center, ensuring that patient and provider interactions are of the highest quality and enabling the diagnosis, treatment, and ongoing management of Parkinson’s disease.
The clinic utilizes a state-of-the-art electronic medical record system to track and monitor patients’ physical and psychosocial status, as well as caregiver burden, mood, and quality of life. This approach gives clinicians, patients, and caregivers unprecedented information on the progression of disease and the effectiveness of their treatment regimen.
This health care delivery model will be shared and can be replicated in outpatient offices across the nation to enhance the lives of people living with Parkinson’s disease. The clinic’s mission aligns with The Parkinson Council’s mission to improve the quality of life for patients and their caregivers, and educating patients, caregivers, and health professionals about Parkinson’s disease.
Article by Diane Kukich
Photos by Kathy F. Atkinson